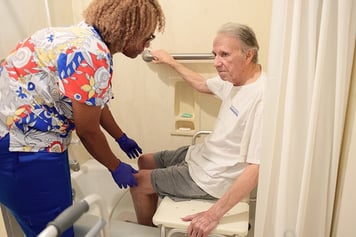
When you ask Google to define a fall, the definition is simple: it’s an event which results in a person coming to rest inadvertently on the ground. After 30 years practicing as a physical therapist, I know that a fall is much more than this definition.
A fall can affect an entire lifestyle, daily functions and overall emotional well-being. One in three elderly adults fall each year and the chance of a fall increases every year2.
Here’s how one of my patients, Hannah, who also happens to be an MD, describes it: “My greatest fear in life is falling and becoming bedridden. I’m more afraid of falling and having a serious head injury or head fracture and spending my last days in bed than dying itself. Being bedridden after a fall doesn’t just rob you of mobility, it robs you of the connection to others that motion facilitates.”
Falls can trigger a vicious cycle of events. Once the nesting phase is reached, it’s a quick progression into depression and lack of confidence that leads to a general weakening which inevitably leads to more falls.
“The first thought down on the floor is, “Am I okay? Did I break any bones? Can I get up from the floor by myself? Will people yell at me for being inattentive and careless? Will they be frustrated and lack sympathy, making everything worse,” says Hannah.
Physical therapists work to break this cycle by intervening before the nesting phase creates a false sense of safety with the patient.
[callout 1]
The average adult has two to three chronic conditions that contribute to a higher risk of falls. The most elderly have as many as 10 contributing conditions. While we think that with old age comes decline and weakness, poor endurance, dizziness and falling, this doesn’t have to be the case.
Physical therapists can be integral in helping the elderly build confidence and feel self-assured in their ability to perform daily functional activities with improved balance and postural stability, thus reducing the fear of falling.
“At their best, the physical therapist will come to see you for who you are and recognize your desire and ability to still live productively in the world,” said Hannah. That therapeutic alliance between your physical therapist and patient may prevent falls and bring longevity and joy for many years to come.”
They do this by leveraging progressive fall reduction programs, which can develop momentum toward building confidence in one’s abilities, strengthen leg muscles and introduce community activities to prevent falls, if introduced early enough. Adhering to these programs can change and improve an aging adult’s life, but buying into this daily lifestyle change of strengthening, becoming more flexible and balanced with exercises is key. Committing to the program helps prevent the mind from hazing over and lifts the spirit to move all while decreasing the fear and ill effects of falls.
“My physical therapist comes twice a week, a voice of reason and reality,” says Hannah. “I listen to her and when I follow her instructions, my legs get stronger. I develop reflexes for not falling backwards, I learn to catch myself in a fall. I think more about what I’m doing when I navigate the hall to the bathroom in the middle of the night. For you see, she teaches me little tricks to prevent slipping and sliding. She teaches me that falls are preventable. She’s shown me the benefits of moving and helped me realize the uselessness and futility of being bed-locked in deceptively soft pillows with the mindless drowning of the TV.”
Modern neuroscience tells us that the brain is capable of repair, recovery and adaptation, and it is movement, or exercise, and repetition that stimulate brain function, even growing new neural connections to bypass the injured ones.
Find out whether you might be a fit for home health care with our home health care assessment quiz.
Paula Giannaras is a physical therapist for Amedisys in Elkton, Maryland.
References:
- Heitzman, Jill. “Geriatric Pharmacology: PT Role and Responsibilities: 3488: Geriatrics: Home Health: Pharmacology.” com, 2019,www.physicaltherapy.com/pt-ceus/course/geriatric-pharmacology-pt-role-and-3488.
- Lowry, Meg. “Balance Training with Smart Phone Apps and Household Items: 3298: Geriatrics: Home Health: Orthopedics.” com, 2019,www.physicaltherapy.com/pt-ceus/course/balance-training-with-smart-phone-3298.
- Studer, Mike. “Why This Test? Clinical Decision Making for Balance: 3185: Geriatrics: Home Health: Neurology: Orthopedics.” com, 2018,www.physicaltherapy.com/pt-ceus/course/why-this-test-clinical-decision-3185.