Many older adults prefer to get their healthcare at home, if possible. With excellent home health coverage under Medicare, Medicaid and many private insurance plans, people are anxious to take advantage of Medicare’s Home Health Benefit. Usually the question is, “Am I eligible for home health?” Ultimately your doctor makes this determination, but the process may be easier if you understand Medicare’s home health coverage and home health criteria.
Adults 65 and older, and some individuals who otherwise qualify for benefits, meet the Medicare home health requirements detailed below.
[callout 1]
1. Your doctor orders home health care for you
To determine if you meet home health eligibility criteria, your doctor will meet with you to evaluate your needs. Some of the signs you may be eligible for home health care include a new diagnosis or worsening of an existing condition, a new medication or change in medication, or frequent visits to your doctor or hospital.
When you meet with your doctor, they will consider:
- Do you need intermittent (not continuous) skilled nursing, physical therapy or speech therapy, or ongoing occupational therapy? Intermittent can be as often as daily in certain circumstances, or as little as every 60 days. The main point is you won’t need regular, long-term care.
- Which home health services are medically reasonable and necessary?
2. You’re considered “homebound,” or confined to your home
To be eligible for home health, you also need to meet the Medicare homebound criteria. Essentially, this means it’s very difficult for you to leave home and you need help to do so. Your doctor will evaluate how you’re doing to decide if you meet Medicare’s homebound criteria. They’ll likely certify that you’re homebound if:
- You need the help of a supportive device (cane, walker, wheelchair, etc.) or another person to get out of the house OR your doctor believes your illness could get worse if you leave home.
- It takes a great deal of effort for you to leave home, so:
- You don’t leave home often; and
- If you do leave home, it’s for a short time and to do something you really need to do. For example, you generally can:
- Visit your doctor or get medical treatment
- Get a haircut or visit the beauty parlor
- Attend religious services
- Go to a licensed or accredited adult daycare
- Attend an important event like a wedding, family reunion, graduation or funeral
3. You receive care from a Medicare-certified home health care agency
Home health agencies must meet certain federal requirements to get certified by Medicare. To find a certified home health agency and compare quality scores among different providers, visit Medicare’s Care Compare website.
How Does Home Health Care Eligibility Work?
The Medicare home health benefit can be hard to understand. Here are a few real-world examples so you can see how it works in people’s lives:
- John fell in his bathroom and needed hip surgery. He spent five days in the hospital and is ready to be discharged, but he hasn’t fully healed. In his discharge paperwork, John’s doctor includes information about being homebound and needing short-term skilled care. His doctor lists the services and equipment John will need. John is eligible for home health care.
- Michael has ALS. His balance is getting worse, so he uses a cane to move around. It takes him hours to get dressed and ready for the day. By the time he’s done, he’s too tired to do much else. He leaves his house periodically to go to church, medical appointments, weekly support group meetings and special family celebrations, but he needs help to do so and is often worn out afterwards. For his safety, he needs constant assistance, but his spouse works and can only care for him a few hours per week. On a recent visit, his doctor ordered home health care, including physical therapy, occupational therapy, skilled nursing and a home health aide. Michael meets Medicare’s home health eligibility criteria.
- Janet is a 75-year-old with heart failure. Her daughter drives her to see her doctor and she’s usually so tired when she gets home that she sleeps for an hour and then rests for the remainder of the afternoon. “Every time I go someplace, I am just worn out when I get home,” she says. “I don’t know what I would do if my daughter could not go with me to help.” During her last visit with her doctor, she asked about home health care. Her doctor determined she meets the home health requirements and referred her to a local agency.
Eligibility Checklist
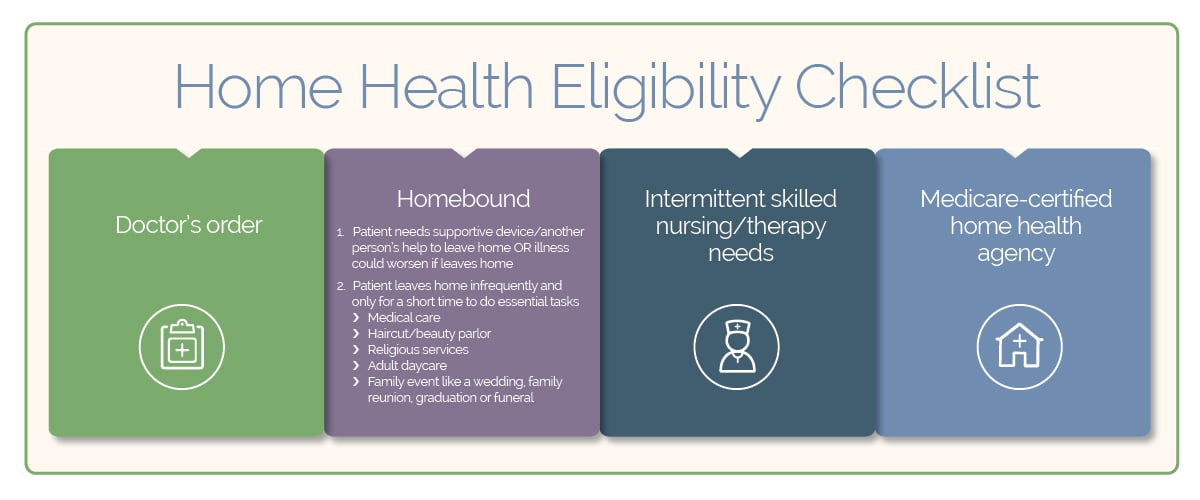
If you’re eligible for the Medicare home health benefit, your doctor will document your needs and sign a home health certification. They’ll also need to review and sign your plan of care at regular intervals. Some of the services that may be available to you include skilled nursing care, medical social services, help with daily activities from a home health aide, medical supplies, and speech, occupational and physical therapy.
If you’re interested in exploring your home health benefits, talk to your doctor. You can also call an Amedisys home health care center near you to learn more about home health care eligibility and our services.






