Medicare is a federal health insurance program that serves as a vital support system for people aged 65 and older. Patients may be eligible for Medicare earlier if they have certain disabilities, end-stage renal disease or amyotrophic lateral sclerosis (ALS). Among Medicare’s unique benefits is home health care, which provides skilled nursing, therapies and other care services to those with specific health needs.
What is Home Health Care?
Home health care is when medical care comes to you — right in your own home. It’s designed for people who are recovering from an illness, surgery, or injury, or dealing with a chronic condition, and are homebound. The goal is to help you stay safe and comfortable at home and avoid an unnecessary trip back to the hospital.
It can include things like:
- Skilled nursing care (like wound care, IV therapy or monitoring vital signs)
- Physical, occupational or speech therapy
- Help managing medications
- Assistance with personal care, like bathing or dressing if medically necessary
- Health education for you and your caregivers
It doesn’t usually cover:
- Housekeeping or cleaning services
- Meal preparation (unless it's part of a medical plan)
- Transportation to appointments
- Errands or non-medical companionship
- 24-hour care — home health care is intermittent. Continuous, round-the-clock care is not provided.
- Oral medication administration
If you're ever unsure whether a service qualifies, it's a good idea to check with your doctor or home health provider — they can help sort out what’s covered and what’s not.
Basic Eligibility for Medicare Home Health Care Benefits
To be eligible for Medicare home health care benefits, you must meet several key criteria that help determine if your condition warrants home health care benefits. 1
Medicare Part A
- Covers most home health skilled care services, even if you haven’t been hospitalized.
- You may qualify if:
- You’re homebound (can’t leave home easily).
- You need skilled nursing or therapy (not just help with daily tasks).
- Your doctor certifies your need and creates a care plan.
- No hospital stay required.
- No deductible or coinsurance for covered home health services.
Understanding the Basic Home Health Eligibility Criteria
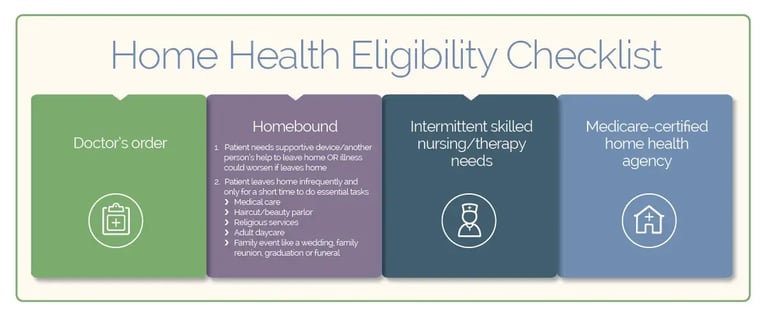
Let’s take a closer look at the eligibility criteria:
1. Being Homebound
You are considered homebound if it's very hard for you to leave your home, or if your doctor advises against going out because of your health. This could be due to things like a disability, recovering from surgery, a serious illness or memory problems. Your main doctor decides if you meet this condition based on your physical and medical needs.
2. Demonstrating a Medical Need
In addition to being homebound, you must require intermittent skilled nursing care or skilled therapy services.
3. Physician Approval/Face-to-Face Encounter
Your physician must authorize home health care services and review your care plan regularly.
You must have a required face-to-face encounter with your physician within the timeframes required by Medicare. The encounter must also be related to the primary reason you need home health care. 2
4. Care is Provided by a Medicare-Certified Home Health Agency
The agency providing care must be certified by Medicare.
Common Conditions Among Patients Requiring Home Health Care
Home health care services can support many conditions commonly experienced by patients aged 65 and above.
A few of these include:
- Congestive heart failure, hypertension and other heart conditions
- Diabetes and accompanying issues
- Chronic obstructive pulmonary disease (COPD) and other lung conditions
- Stroke
- Cancer
- Recovery from knee or hip replacement surgery or other orthopedic procedures
- Wounds related to pressure injuries or other conditions
- Chronic kidney disease
- Dementia, Alzheimer’s disease or Parkinson’s disease
A home health care plan tailored to your needs can help address these conditions, providing needed support to promote well-being, independence and quality of life for you while helping to avoid unnecessary hospital stays.
Why Would a Person be Discharged from Home Health Care?
Several things can change your basic eligibility and lead to the termination of home health care. These factors include:
- No longer homebound: Your health improves enough to leave home safely and leaving home is no longer a taxing effort.
- No longer needs skilled care: Nursing or therapy services are no longer medically necessary.
- Health goals met: You complete the care plan and reach recovery goals.
- Patient chooses to stop: You decide to end home health services.
Types of Care Covered Under Medicare Home Health Care
Medicare home health care provides a wide range of skilled nursing, therapy and support services to address the medical and therapeutic needs of eligible patients depending on their needs.
Skilled Nursing Care
Skilled nursing care includes:
- Observation and assessment: Skilled services provided by a nurse when a patient's condition requires close monitoring to detect changes that only a licensed nurse can identify due to the complexity or instability of the condition.
- Hands-on care: Nurses perform skilled tasks like wound care, catheter care, tube feeding, injections, and other medical treatments. Nurses may also teach patients and caregivers to perform the care themselves.
- Teaching and training: Nurses teach patients and their caregivers how to take care of health needs at home. By sharing knowledge and building confidence, they help patients take charge of their recovery and stay involved in their care. This is called empowerment and patient activation—it means the patient is in control of their health, with expert support along the way.
- Medication administration: Nurses give injections and infusions (not pills), as prescribed. Nurses may also teach patients and caregivers to administer medications themselves.
- Psychiatric nursing: Agencies like Amedisys may offer psychiatric nurses trained to support mental health needs in some locations.
Therapy Services
Therapy services include:
- Physical therapy, which helps patients manage pain and regain strength and mobility and reduce fall risk
- Speech therapy, which helps with swallowing difficulties and communication challenges.
- Occupational therapy, which helps patients regain or improve everyday skills like bathing, grooming, dressing, and other self-care tasks. Occupational therapists also assess the patient’s home setup and suggest changes to help prevent falls and make everyday activities safer.

Additional dependent services are available once a patient has a qualifying need for skilled nursing or skilled therapy services, including:
- Home health aides: When assistance is needed as part of the overall home health plan, aide services assist the patient with hands-on personal care.
- Medical social work services: Social workers help resolve social or emotional problems that impact a patient’s recovery or treatment plan.
Supplemental Services Outside of the Medicare Home Health Care Benefit
Medicare pays for basic home health care services, but there may be other helpful services that Medicare doesn’t cover. These extra services — like help at home or in your community — can depend on where you live and the rules of the program. To qualify, you’ll need to be evaluated, and your doctor or a social worker must approve the services.
Services like these include:
- Meals on Wheels
- Homemaker services
- Housekeeping
- Shopping assistance
These non-medical services are typically funded through out-of-pocket payments or community resource programs. Patients eligible for Medicaid or Veterans Affairs (VA) benefits may receive additional support. To find out more, contact your insurance plan or a home health care agency that connects patients with these external resources.
Costs for Medicare Home Health Care
Understanding home health care costs is crucial for patients and their families when deciding to elect Medicare home health services. It’s always important to fully understand the cost of benefits from your agency of choice, but the following key points are a great place to start:
No Out-of-Pocket Costs for Medically Necessary Services
For eligible patients, Medicare covers the costs of all home health care services deemed necessary by the physician, ensuring that these patients do not have to pay out of pocket. 3
Transparency in Medicare Coverage
The home health care agency is responsible for informing the patient of all costs associated with Medicare coverage. This level of transparency allows patients to plan and manage their healthcare expenses.
Partial Responsibility for Medical Equipment
When a patient requires Medicare-covered medical equipment, Medicare Part B may be responsible for covering 80 percent of the cost, and the patient will be responsible for the 20 percent copay. It’s important to work with the medical equipment provider to receive an estimate to help anticipate and manage out-of-pocket expenses. 4

Next Steps for Home Health Care
If you or someone you care about has a serious or long-term illness, talking openly and acting quickly can make a big difference in getting the right care and support.
Take these recommended next steps if you think home health care may be the right choice:
1. Facilitate open communication.
If the care is for a loved one, encourage them to share their wishes and desires with you and other family members and caregivers. Make sure everyone involved is aware of your or your loved one’s goals for care.
2. Contact an agency for connections to resources.
A reputable agency can help you access the right resources. In addition to offering access to needed services, the right agency can provide comprehensive support with questions and make sure the entire experience is seamless.
3. Consider agencies with a full continuum of care.
A full continuum of care provides a full range of healthcare services that address a person’s care needs across different stages of illness or recovery.
Choose an agency that offers a full continuum of care — not just home health care services — so you or your loved one can smoothly transition from one program to another, if necessary. This approach ensures they receive consistent, uninterrupted care tailored to their needs.

Ready to Take the Next Steps for Home Health Care?
Severe or chronic illnesses create many challenges, but navigating Medicare home health care benefits shouldn't be one of them. At Amedisys, we’ve been offering high-quality care since 1982 and are a leading provider of healthcare in the home. Our home health experts are available to help answer any questions you may have about eligibility and how to start care. Contact us today using the form below or call a location near you.
Melanie Morris, MBA, MSN, RN, COS-C is the Assistant Vice President of Care Delivery Management for Amedisys. In her 28 years as a nurse, she has enjoyed caring for many types of patients and is passionate about providing holistic care to patients in their homes, especially those with chronic conditions such as wounds.





